 Atelectasis, obesity, elderly and underlying structural lung disease could be the predisposing factors for rapid deterioration in the clinical condition. 1,2 COVID-19 patients faced slow onset severe hypoxemia with hypocapnia. Intra-pulmonary shunting, relatively preserved lung complian-ce, lack of excessive dead space, lack of substantial pulmonary embolism or microvascular thrombosis and dysfunctional hypoxemic vasoconstriction are the key features. 1-2 Patients often presents in stable condition where they are able to speak full sentences with oxygen saturation of 80%, hence pulse oximetry may be a marker for respiratory dist-ress. With normal lung compliance and many of them not in respiratory distress, hypoxemia does not correlate with their clinical condition. 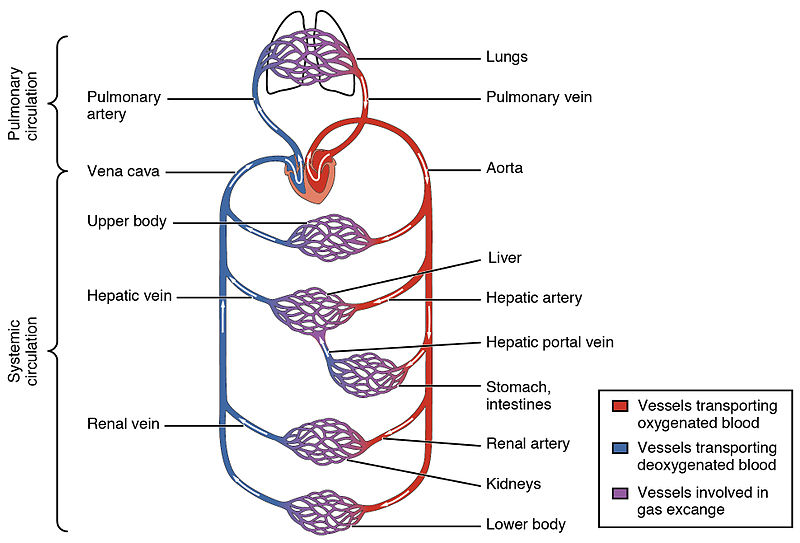
1,2 The disease process is been treated as acute respiratory distress syndrome (ARDS) but it is not typical ARDS. COVID-19 made us to think about this forgotten approach.ĬOVID-19 lung injury includes viral medial inflammation, alveolar epithelial dysfunction, impaired surfactant, alveolar collapse, and increased pulmonary artery pressure patients. Silent hypoxemia can last forever but individuals could present to a healthcare facility with this condition occasionally. 1 It applies to any lung pathology which causes a reserved amount of shunt while saving the rest of the lung such as lobar pneumonia or atelectasis. 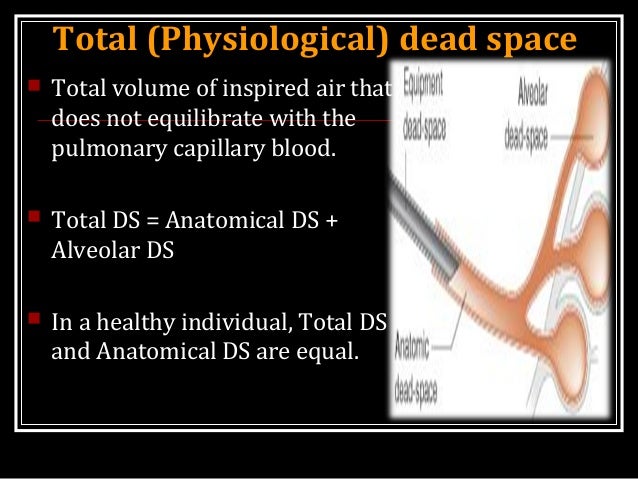
With Coronavirus disease of 2019 (COVID-19) pandemic, silent hypoxemia (significant hypoxemia without dyspnea) is a phenomenon to understand with associated shunt physiology, preserved lung compliance, and lack of dead space. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
